What Causes Sudden Hair Shedding?
Hair shedding can be alarming—but not all hair loss is permanent. If you’ve noticed more hair strands in the shower, floor, or your brush, it could be telogen effluvium (TE)—a temporary form of hair loss often triggered by physical or emotional stress, illness, or other lifestyle imbalances.
Telogen effluvium is the second most common cause of hair loss in women, especially between ages 30–60. It occurs when a large percentage of your hair suddenly shifts from the growth phase (anagen) into the resting phase (telogen), leading to excessive shedding.
What Happens in TE?
- Normally, you shed around 10% of your hair each day (roughly up to 100 hairs).
- In TE, that number can spike to more than 20-25% (300–500 hairs), often in clumps.
You may notice:
- Hair all over the shower, bathroom floor, or pillow
- Thinner ponytail
- Widening midpart line
- Hair “falling out in handfuls”
- Trichodynia: Some patients feel burning, stinging, or tenderness in the scalp—this is inflammation-related and temporary.
This temporary hair shedding condition usually becomes noticeable a few weeks to three months after the triggering event. The acuity and extent of shedding can depend on the severity and duration of the stressor(s). Typically, hair shedding lasts for less than six months and does not result in total hair loss.
What to Expect with Telogen Effluvium (TE)
Hair loss from TE occurs after a trigger pushes follicles prematurely into the resting (telogen) phase.
- Shedding from telogen effluvium typically begins 6–12 weeks after the triggering event, but can start sooner.
- It often lasts 3–6 months before tapering off, assuming the body rebalances.
- The good news is that telogen effluvium is often reversible, once the stressor(s) is found and removed or treated.
- However, prolonged shedding (lasting more than 6 months) or visible thinning could suggest another underlying issue, like AGA or chronic telogen effluvium (CTE).
Diagnosing TE
Accurate diagnosis includes:
- Hair loss history (onset, severity, pattern)
- Review of medical history, medications/supplements, nutrition, hair care practices, and lifestyle factors
- Scalp and hair physical exam
- Comprehensive lab testing
- Scalp biopsy (if unclear or persistent)
Keep in mind: TE often overlaps with androgenetic alopecia (AGA)—a genetic hair loss condition. While androgenetic alopecia is the most common type of hair loss in men and women and tends to worsen with age, episodes of TE can occur alongside it, potentially activating or exacerbating the genetic hair loss.
TE vs. AGA
| Telogen Effluvium (TE) | Androgenetic Alopecia (AGA) |
|---|---|
| Sudden, excessive shedding | Gradual thinning and miniaturization |
| Diffuse across the scalp | Patterned (temples, crown) |
| Often linked to a specific trigger(s) | Progressive and genetic |
| No visible scalp inflammation | Follicles miniaturize over time |
| Good chance of full regrowth | Long-term treatment often needed |

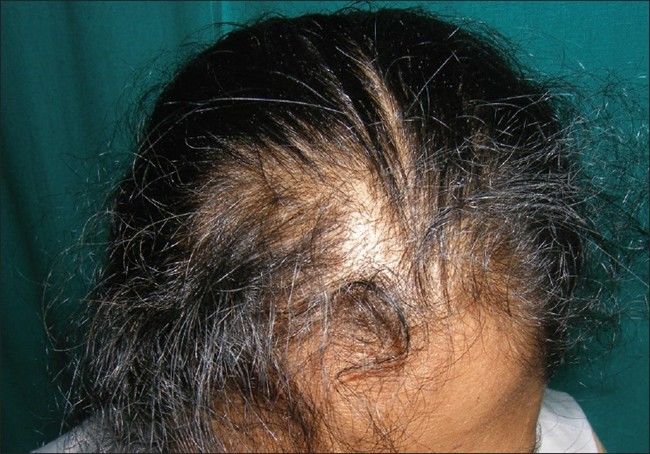
Trichoscopy shows visible dilated blood vessels (capillaries), several regrowing hairs, an increased number of follicular units with one terminal hair, empty follicles, and decreased hair density.

What Are Common Causes of Telogen Effluvium?
Let’s break down the most common causes of TE—and what you can do about them.
Physical or Emotional Stress
Stress is one of the most recognized causes of telogen effluvium. But not all stress is created equal.
Major Triggers:
- Surgery, anesthesia, illness, or trauma
- Profound emotional events like:
- Death of a loved one
- Divorce or relationship problems
- Job loss or financial pressure
- A new medical diagnosis affecting you or a loved one
- Mental health disorders
- People with severe hair loss are more likely to experience psychological challenges than those with mild hair loss
- Studies show that individuals with hair loss are at an increased risk of psychiatric conditions such as major depressive episodes, anxiety disorders, personality disorders, social phobia, or even paranoia
- One study found that women under intense stress were 11 times more likely to experience hair loss
- The stress caused by losing hair can intensify the shedding, making it harder to pinpoint whether stress is the cause of hair loss or a response to it. Breaking the cycle is key to recovery
Hormonal Changes
Hormones strongly influence hair growth. Sudden hormonal shifts can throw your hair cycle off balance.
Postpartum Hair Loss
During pregnancy, there is a rise in estrogen and progesterone levels, resulting in fewer hairs being shed and more hair accumulating in the active growing (anagen) phase. This results in thicker and denser hair. After delivery, estrogen and progesterone levels return to their pre-pregnancy levels, disrupting the balance between growing and shedding hairs again.
Hair shedding typically begins within a few weeks to 3 months after childbirth, and the hair eventually grows back within 12 months, but it may look different. The new hair may exhibit changes in texture, color, or characteristics (e.g., curly), and it may not grow to the same length as it did previously. These changes are a normal part of the regrowth process and can vary from person to person.
If the hair does not return, it may be a possible sign that this event triggered the activation of androgenetic alopecia (female pattern hair loss) or that other triggers for TE are causing continued thinning and shedding (e.g., nutrient deficiencies, thyroid disorders, elevated blood sugar).
Postpartum nutrient depletion is very common and can significantly impact recovery, mood, energy, hair health, and hormonal balance. Here’s a breakdown of key nutrients often depleted after pregnancy and their estimated prevalence in postpartum women:
Commonly Depleted Nutrients After Pregnancy
Iron
- Why: Blood loss during delivery and increased demands during pregnancy.
- Prevalence: ~25–50% of postpartum women experience iron deficiency; higher in those with heavy bleeding or closely spaced pregnancies.
- Signs: Fatigue, hair loss, brain fog, shortness of breath.
Vitamin B12
- Why: Used heavily during fetal development; may be lower in those with low intake or GI issues.
- Prevalence: Up to 30% of postpartum women may have low or borderline B12.
- Signs: Fatigue, depression, memory issues, tingling.
Folate (B9)
- Why: Rapid cell division during pregnancy depletes stores.
- Prevalence: ~20–25%, especially if not continuing prenatal vitamins.
- Signs: Fatigue, anemia, mood swings.
Vitamin D
- Why: Common deficiency in the general population; needed for fetal bone development and immune regulation.
- Prevalence: Up to 80% of postpartum women may be insufficient or deficient.
- Signs: Fatigue, low mood, muscle aches, hair loss.
Zinc
- Why: Needed for fetal growth, tissue repair, and immune function.
- Prevalence: ~30–50% postpartum deficiency is estimated.
- Signs: Poor wound healing, weakened immunity, hair thinning.
Magnesium
- Why: Used in over 300 enzymatic reactions; stress and hormonal shifts increase needs.
- Prevalence: ~40–60% in U.S. adults; may be higher postpartum.
- Signs: Anxiety, sleep issues, muscle cramps, constipation.
Omega-3 Fatty Acids (EPA/DHA)
- Why: Depleted due to fetal brain development; low intake post-pregnancy worsens status.
- Prevalence: High, especially in women who don’t eat fatty fish or supplement.
- Signs: Mood swings, brain fog, dry skin/hair.
Iodine
- Why: Essential for thyroid function and brain development; often not repleted postpartum.
- Prevalence: Up to 35% of U.S. women have inadequate iodine intake postpartum.
- Signs: Fatigue, thyroid dysfunction, cold intolerance.
Calcium
- Why: Transferred heavily to fetus and breastmilk; demand spikes during lactation.
- Prevalence: Many women fail to meet daily intake (especially if dairy-free).
- Signs: Bone/joint pain, brittle nails, muscle cramps.
| Nutrient | Depletion Rate | Why It’s Depleted | Key Symptoms |
| Iron | 25–50% | Blood loss, fetal demands | Fatigue, hair loss |
| B12 | Up to 30% | Cellular growth, low intake | Fatigue, brain fog |
| Folate | ~25% | Fetal needs, DNA synthesis | Anemia, mood changes |
| Vitamin D | Up to 80% | Low sunlight, high demand | Low mood, fatigue |
| Zinc | 30–50% | Fetal growth, immune shifts | Hair thinning, low immunity |
| Magnesium | 40–60% | Stress, hormonal shifts | Sleep issues, anxiety |
| Omega-3s | ~50–70% | Brain development drain | Mood changes, dry skin |
| Iodine | Up to 35% | Thyroid support, breastmilk needs | Cold intolerance, fatigue |
| Calcium | Common | Bone/milk transfer | Muscle cramps, bone pain |
Birth Control-Induced Hair Shedding
Birth control pills work by altering your body’s natural hormone balance to prevent ovulation. These shifts can impact the hair growth cycle, especially if your body is sensitive to hormonal changes.
This usually occurs due to:
- Hormone fluctuations that disrupt your hair’s natural growth cycle.
- A drop in estrogen, which normally helps keep hair in the growth (anagen) phase.
- Sensitivity to progestins (synthetic progesterone) in certain birth control pills, which can mimic androgens (male hormones) and negatively impact hair follicles.
This imbalance can trigger or exacerbate female pattern hair loss (FPHL) or Telogen Effluvium.
Starting Birth Control
When you start the pill, your body needs time to adjust to the new hormonal environment. This hormonal shift can temporarily shock your hair follicles, causing more strands than usual to enter the telogen (shedding) phase.
Stopping Birth Control
When you stop taking the pill, your natural hormones may fluctuate dramatically before stabilizing. This rapid change can also trigger telogen effluvium, even if you didn’t have hair loss while on the pill.
Think of it like a seesaw: any abrupt hormonal drop or spike can throw off your hair’s rhythm.
What You Can Do
- Stay consistent: Avoid frequently switching birth control types or stopping and restarting, which can confuse your hormonal balance.
- Support your body: Eat nutrient-rich foods, manage stress, and ensure you’re not iron or vitamin D deficient.
- Consult an expert: A hair loss specialist can determine if your shedding is due to telogen effluvium or something else and guide you toward a plan that supports regrowth.
IVF and Hair Loss: Understanding the Connection
Patients undergoing in vitro fertilization (IVF) often face challenges beyond the emotional and physical stress of fertility treatment. One concern that doesn’t get enough attention is hair loss linked to IVF hormone therapy.
Why IVF Can Trigger Hair Loss
Hormone fluctuations
IVF treatments rely on strong doses of estrogen and progesterone to stimulate the ovaries. These sudden hormonal shifts can disrupt the hair growth cycle, pushing more hairs into the telogen (shedding) phase. This type of shedding is called telogen effluvium.
Androgen sensitivity
In women who carry a genetic predisposition for androgenetic alopecia (female pattern hair thinning), fertility medications may accelerate the process. Certain hormones can increase the activity of androgens on the hair follicle, triggering visible thinning at the crown or widening of the part line.
Physical and emotional stress
The IVF process itself—frequent procedures, high stress, and lack of sleep—adds another layer of strain. Stress is a well-known factor in shifting hairs into premature shedding phases.
The Emotional Impact
Patients undergoing IVF also report significant distress over hair loss related to hormone treatments. A recent study by Kamili et al. revealed a subset of patients who considered halting fertility treatment specifically because of hair loss. As IVF use rises globally, this problem will likely become even more of a concern.
Hair loss during IVF isn’t just cosmetic—it can add to the emotional toll of an already difficult journey. Many women describe it as another reminder that their body feels “out of control.”
Moving Forward
The good news is that IVF-related hair loss is often temporary, especially in cases of telogen effluvium. Once hormones stabilize after treatment, hair shedding usually improves within several months. For patients with underlying androgenetic alopecia, early evaluation and tailored treatment with a hair loss specialist can make a big difference in slowing progression and restoring confidence.
Thyroid Disorders
Hypothyroidism (Underactive Thyroid)
What Happens
When your thyroid hormones slow down, your body’s systems, including your hair growth cycle, lose momentum. Hair follicles enter the resting (telogen) phase too early, leading to excessive shedding.
When unbalanced, around 33% of people with hypothyroidism experience noticeable hair loss.1
Why it Matters
Treatment with thyroid hormone helps restore your normal hair cycle—and your hair can grow back.
Your thyroid doesn’t just regulate your energy and metabolism—it plays a major role in your hair’s health and appearance.
Research published in the Journal of Clinical Endocrinology & Metabolism showed that thyroid hormones also affect the cells responsible for hair color. Low levels can lead to early graying or whitening of the hair, even in younger individuals.
Hashimoto’s Thyroiditis (Autoimmune Hypothyroidism)
What Happens
This condition involves the immune system attacking your thyroid. The resulting inflammation and hormone imbalance can trigger telogen effluvium, and autoimmune flare-ups can further disrupt hair growth.
Nutrient deficiencies can also occur in Hashimoto’s such as:
- Low ferritin (iron stores) – Ferritin < 70 ng/mL is linked to hair loss.
- Low zinc – Essential for hair growth and immune function.
- Low vitamin D – Affects hair follicle cycling and immune regulation.
- Low vitamin B12 – Can impair red blood cell function, reducing oxygen delivery to hair follicles.
Hashimoto’s affects about 2% of people, but hair loss is a common symptom. 2
Why it Matters
Controlling inflammation, normalizing thyroid hormone levels, and addressing any nutritional deficiencies can help hair regain its usual thickness.
Aside from TE, What Type of Hair Loss Does Hashimoto’s Cause?
- Androgenetic Alopecia (Female or Male Pattern Hair Loss) – Hashimoto’s may worsen genetic hair thinning due to hormonal dysregulation
- Alopecia Areata (Patchy Hair Loss) – In some cases, autoimmune hair loss occurs alongside Hashimoto’s
Hyperthyroidism (Overactive Thyroid)
What Happens
When your thyroid goes into overdrive, your metabolism speeds up, also pushing hair follicles into the telogen (resting) phase too early, leading to hair shedding.
Around 50% of those with hyperthyroidism experience hair shedding. 3
Why it Matters
Treating the thyroid disorder typically calms the overactive hair shedding, allowing hair to recover.
Feeling Off—Even with “Normal” Thyroid Labs?
If you’re dealing with low thyroid symptoms like fatigue, weight gain, brain fog, dry skin, or cold intolerance, but your thyroid labs come back “normal,” you’re not alone.
Many people still experience symptoms of an underactive thyroid even when their lab values are within the reference range.
When “Normal” Doesn’t Feel Right
Standard lab ranges don’t always reflect what’s ideal for everyone. Some people feel best when their thyroid hormone levels (such as TSH, Free T3, and Free T4) are at the upper or lower end of the normal range, rather than somewhere in the middle.
In other words, your numbers might be “technically normal,” but still not optimal for YOU.
What You Can Do
If your symptoms persist, don’t ignore them just because your labs say “normal.” You know your body better than any lab result. Consult with a healthcare provider who adopts a functional medicine approach to thyroid health.
They’ll look at:
- Your full symptom picture.
- Order more than the standard thyroid panel (TSH, T3, T4).
- Review other factors, including nutrient levels, stress, inflammation, and hormone balance.
Insulin Resistance
There is a strong connection between pre-diabetes/diabetes and hair loss, primarily due to hormonal imbalances, inflammation, and poor circulation. Below are the key mechanisms by which pre-diabetes can contribute to hair thinning and loss.
1. Insulin Resistance and Hair Follicle Miniaturization
- Insulin resistance (a hallmark of pre-diabetes/diabetes) occurs when cells become less responsive to insulin, leading to high blood sugar levels.
- Excess insulin stimulates androgen (DHT) production, which can shrink hair follicles and lead to androgenic alopecia (male/female pattern baldness).
- High insulin levels also reduce SHBG (sex hormone-binding globulin), thereby increasing free testosterone and DHT, which are associated with hair follicle miniaturization.
2. Chronic Inflammation and Oxidative Stress
- Insulin resistance leads to chronic, low-grade inflammation, which can trigger the release of inflammatory cytokines that damage hair follicles.
- Oxidative stress increases the production of free radicals, which can lead to follicular damage and premature hair loss.
- Conditions like seborrheic dermatitis and scalp inflammation are more common in individuals with metabolic disorders.
3. Poor Circulation and Reduced Nutrient Delivery
- High blood sugar levels cause damage to small blood vessels.
- Hair follicles require a steady supply of oxygen and nutrients, and poor circulation leads to weaker, thinner hair.
- Small blood vessel disease reduces blood flow, which may contribute to hair loss.
4. Thyroid Dysfunction and Hair Loss
- Insulin resistance is linked to thyroid dysfunction, especially hypothyroidism, which can cause diffuse hair thinning.
5. Nutrient Deficiencies Affecting Hair Growth
- Insulin resistance can deplete key hair-supporting nutrients:
- Iron & Ferritin: Low iron levels can trigger telogen effluvium.
- Vitamin D & Magnesium: Essential for follicle health and insulin sensitivity.
- Biotin & Zinc: Important for keratin production.
6. Stress, Cortisol, and Hair Shedding
- Insulin resistance is often associated with high cortisol levels, which can trigger telogen effluvium (excessive hair shedding).
- Chronic stress worsens insulin resistance and leads to hormonal imbalances affecting hair growth.
Nutritional Deficiencies
Hair is one of the first things your body sacrifices when you’re not getting the fuel it needs. That’s because hair isn’t essential for survival, so when your body senses a shortage of nutrients or energy, it diverts resources to more critical systems like your heart, brain, and immune function.
This shift can push hair follicles out of the growth phase (anagen) and into the shedding phase (telogen), leading to telogen effluvium.
Most Common Nutrient Deficiencies Linked to Hair Shedding:
Low Protein Intake
Hair is composed primarily of keratin, a type of protein. Without enough dietary protein, your body struggles to support the hair growth cycle.
When your protein intake drops too low for too long, the body starts rationing. It deprioritizes non-essential functions, such as hair production, triggering telogen effluvium.
Ensure you’re consuming enough high-quality protein from sources like eggs, chicken, fish, beans, tofu, Greek yogurt, or protein shakes—especially if you’re active or healing from illness.
If you don’t have a nutritionist, use an online protein calculator to help guide you.
Low Folate (Vitamin B9): The Cell Builder
- Folate is needed for cellular growth and repair—especially in fast-growing tissues like hair.
- Low folate levels disrupt hair follicle activity and can trigger premature shedding.
- At risk: Poor diet, alcohol use, gut absorption issues.
Low Vitamin B12: The Oxygen Mover
- Vitamin B12 helps make red blood cells and delivers oxygen to your scalp.
- Low B12 levels can lead to poor oxygen flow to the follicles, resulting in increased hair loss.
- At risk: Vegans, vegetarians, older adults, and gut disorders.
Low Vitamin D: The Follicle Regulator
- Vitamin D supports hair follicle cycling, bone, mood, and immune health.
- Deficiency is linked to AGA, telogen effluvium, and alopecia areata.
- At risk: Low sun exposure, darker skin, sunscreen use, and indoor lifestyles.
Low Iron & Ferritin: Fuel for Hair Follicles
Iron deficiency is one of the top nutritional causes of TE, especially in women. Iron deficiency is the most common nutritional deficiency in the United States, affecting one in three adults. Globally, over 2 billion people are affected by iron deficiency.
Think of iron as the oxygen carrier and ferritin as the storage tank. Low levels mean your hair follicles don’t get the oxygen they need to stay active.
- Low ferritin levels are strongly associated with increased hair shedding, particularly in women.
- Without sufficient iron, your body prioritizes vital organs over hair.
- You can have “normal” ferritin levels and still lose hair if they’re not optimal.
One study found:
- 94.9% of TE patients had low hemoglobin
- 89.1% had ferritin <70 ng/mL
- 64% had ferritin <30 ng/mL
Even if you’re not anemic, low iron stores can disrupt the hair cycle.
People at Risk for Low Iron
Low iron can develop when dietary intake, absorption, or demand doesn’t meet the body’s needs. Common at-risk groups include:
- Vegans and vegetarians: Avoid meat, the richest source of heme iron, which is more easily absorbed than plant-based (non-heme) iron
- Pescatarians: Eat fish but often limited red meat intake, which can still reduce overall iron intake
- People following Mediterranean diets: While generally healthy, these diets emphasize fish, vegetables, and whole grains with minimal red meat — potentially lowering iron intake
- Women of reproductive age: Menstrual blood loss increases iron requirements
- Pregnant women: Iron demand rises significantly for fetal growth and increased blood volume
- Endurance athletes: Increased red blood cell turnover, sweat loss, and GI microbleeds can deplete iron
- Frequent blood donors: Repeated donations reduce iron stores
- People with gastrointestinal disorders: Conditions like celiac disease, IBD, or low stomach acid can impair iron absorption
- Older adults: Reduced dietary intake and absorption efficiency contribute to deficiency risk.
A diet low in red meat or high in iron-blocking foods (tea, coffee, calcium) further increases the risk.
Low Zinc: The Repair Mineral
Zinc is vital for tissue repair, hormone balance, and immune health—all of which are critical for maintaining healthy hair.
- Deficiency can lead to both telogen effluvium and hair shaft weakening
- It also plays a role in regulating the oil glands on your scalp
Low Selenium: The Scalp Defender
Selenium helps regulate your thyroid (which affects hair growth) and reduces oxidative stress in the scalp.
- Low selenium levels can impair hair follicle function.
- Too much selenium (from supplements) can also cause hair loss, so balance matters.
- Very common in people taking Nutrafol or other selenium-
containing supplements
- Very common in people taking Nutrafol or other selenium-
For more information on nutritional deficiencies, please click here.
Rapid Weight Loss or Dietary Changes
Shedding often happens after:
- Crash dieting or calorie restriction
- Eating disorders
- Weight loss surgery
- Weight loss medications (GLP1s- semaglutide, tirzepatide, etc.)
Low Calorie Intake
When You Cut Calories Too Much, Your Hair May Pay the Price
Even if you’re eating “healthy” foods, a calorie deficit that’s too extreme or prolonged can shock your system. Crash diets, very low-calorie diets, and certain fasting regimens can all tip your body into survival mode.
This state of energy deficiency disrupts the hair cycle in several ways:
- It increases cortisol (the stress hormone), which can worsen shedding
- It deprives follicles of the energy and nutrients needed to grow
- It reduces estrogen and thyroid hormone levels, both of which support hair health
- It may deplete critical hair-building nutrients like iron, zinc, and biotin
The result? Telogen effluvium that causes sudden, diffuse shedding—often seen 2–3 months after starting the calorie-restricted diet.
How Weight Loss Surgery Can Cause Hair Shedding
It’s common for patients to notice increased hair shedding in the months after bariatric surgery.
Why It Happens
Surgical Stress
Major surgery shocks the system. Your body temporarily redirects energy away from non-essential functions like hair growth to focus on healing.
Rapid Weight Loss
Losing a lot of weight in a short time can disrupt your hair’s normal growth cycle, pushing more follicles into the resting (telogen) phase.
Nutrient Deficiencies
After surgery, it’s harder to absorb key nutrients that support hair growth – especially:
- Protein
- Iron & ferritin
- Vitamin B7 (Biotin), B9 (Folate), B12, and D
- Zinc
- Selenium
What To Do: Rebuild Nutritional Stores
Your body needs the right building blocks to grow hair again. Focus on:
- Protein: To find out how much protein you need each day, multiply your body weight in pounds by 0.6–1.0 (or in kilograms by 1.2–2.2) depending on your activity level and goals — or use an online protein calculator or consult with a nutritionist for personalized guidance
- Iron & Ferritin: Low iron is a major cause of prolonged shedding. Ferritin should ideally be above 70 ng/mL for healthy hair regrowth.
- Zinc & Selenium: Vital for scalp and follicle health.
- Vitamin D: Low levels are linked to multiple hair disorders.
- Vitamin B12 & Folate: Support cell turnover and growth.
Important: Ask your provider to check a full nutrient panel—not just standard labs. Deficiencies can be subtle and missed.
Medications That May Trigger Shedding
Unfortunately, hair shedding caused by medication has not been extensively investigated.
In most cases, there is another underlying reason for a patient’s hair loss. However, if a medication causes shedding, it typically starts within a few weeks to a few months after starting or changing a dose. Most cases resolve over time, even without stopping the drug.
Possible Medications:
- Antidepressants (SSRIs)
- Mood stabilizers (valproic acid, lithium)
- Blood pressure meds (beta blockers, ACE inhibitors, ARBs, diuretics)
- Blood thinners (heparin, warfarin, Xarelto, Pradaxa, Eliquis)
- Isotretinoin (Accutane) – due to vitamin A overload
- Cholesterol (Zocor, Lipitor, Clofibrate, gemfibrozil)
- Lesser chance with Crestor and Lescol
- Gout (Allopurinol)
- Osteoporosis (several bisphosphonates – Fosamax, Actonel, Boniva, and Reclast)
- Antifungals (high-dose fluconazole)
- Chemotherapy – causes anagen effluvium
Can GLP-1 Medications Cause Hair Loss?
Yes—and no.
GLP-1 receptor agonists (like Ozempic®, Wegovy®, Mounjaro®) don’t directly damage hair follicles. But…
- Rapid weight loss shocks the body. This stress can push more hair follicles into the “resting” (telogen) phase.
- Nutrient absorption may drop with lower calorie intake, affecting hair-supporting nutrients like protein, iron, zinc, and B vitamins.
- Hormonal shifts and metabolic changes can further disrupt the normal hair cycle.
Your body is smart—it protects your brain, heart, and muscles first. Hair growth can wait.
What To Do: Nourish From Within
Hair needs fuel. That means:
- Protein: Aim for at least 60–80g daily (more if advised).
- Iron/Ferritin: Ferritin under 70 ng/mL is linked to prolonged shedding.
- Zinc & Selenium: Vital for follicle strength and scalp health.
- Vitamin B12 & Folate: Help regenerate fast-growing cells like hair.
- Vitamin D: A common deficiency in those on GLP-1s, linked to hair thinning.
Important: Ask your provider for a nutrient panel. Many deficiencies are subtle—and easy to miss without testing.
Medication-induced hair shedding is usually temporary and reversible once the drug is stopped or adjusted.
If you’re experiencing unexpected hair loss and started a new medication within the past 6 months, let your provider know—they might help you switch to a safer option or support regrowth with treatments like topical minoxidil.
Chronic Illness
Ongoing inflammation, immune activity, or nutrient issues can disrupt the hair cycle.
Common Conditions Linked to Hair Loss:
- Anemia (aim for hemoglobin >13.0 g/dL)
- Autoimmune diseases:
- Hashimoto’s, psoriasis, lupus, Crohn’s, Sjögren’s, scleroderma
- Chronic infections or inflammatory conditions
- Celiac disease
Scalp Inflammation
When the scalp is inflamed, hair follicles can’t function properly.
Common Causes:
- Poor hygiene (infrequent washing or significant plaque and oil buildup)
- Seborrheic dermatitis
- Scalp psoriasis
Environmental and Lifestyle Factors
- Heavy metals (lead, mercury, arsenic, thallium)
- Harsh styling practices (tight hairstyles, chemical treatments, excessive heat appliances)
- Prolonged sun exposure on the scalp
Treating Telogen Effluvium: What Works and Why
When it comes to telogen effluvium (TE), the first and most important step is figuring out what triggered it. Whether it’s a recent illness, a big life change, or a nutritional deficiency—removing or correcting the cause is key to stopping the shedding and starting regrowth.
Step 1: Identify and Address the Root Cause
Hair shedding won’t stop until the trigger(s) is resolved. That could mean:
- Correcting vitamin, mineral, and hormonal imbalances
- Managing emotional stress or sleep issues
- Adjusting medications or diet (especially after weight loss surgery or stopping birth control)
Once the cause is under control, hair shedding usually slows down—and regrowth typically begins within 3 to 6 months, with visible improvement over 6 to 12 months.
Step 2: Support the Hair Regrowth Process
Even after the stressor is gone, it takes time for hair to recover. These proven treatments can help jumpstart regrowth and boost density:
- Topical or Oral Minoxidil: Encourages follicles to re-enter the growth phase faster and helps speed up recovery.
- Platelet Rich Plasma (PRP) Therapy: Injections of your own concentrated growth factors have been shown to improve hair thickness and regrowth in women with TE.
- Low Level Laser Therapy (LLLT): Safe, at-home red light devices may help boost follicle function and support the regrowth cycle.
- Nutritional Support: balanced diet rich in protein, omega-3 and omega-6 fats, vitamins, and minerals, is essential to feed your growing follicles.
Step 3: Be Patient—Hair Growth Takes Time
It can take 3–6 months for shedding to stop and 6–12 months for visible fullness to return. Hair grows slowly—from deep in the scalp up to the surface—so results are not immediate.
Step 4: Ongoing Monitoring and Support
Regular follow-ups help track progress, tweak treatments, and give you the reassurance that regrowth is happening—even if it’s slow.
Telogen effluvium is temporary, treatable, and reversible in most cases. The earlier you identify the cause and support recovery, the better the outcome.
Chronic Telogen Effluvium (CTE)
If shedding lasts 6+ months, it may be CTE. It often starts like TE but continues—sometimes for years.
- Common in healthy women 30–60
- Similar to TE, CTE is often preceded by a triggering event
- The workup and treatment plan are the same as with Telogen Effluvium (TE)
Several studies have shown that associated factors included nutrient deficiencies:
- 23% had low ferritin levels 4
- 35.7% had low vitamin B12 5
- Trace elements such as zinc and copper are significantly lower in women with CTE compared to healthy individuals 6
- In 33% of cases, no specific cause can be identified, but iron deficiency anemia is frequently implicated as a contributing factor. 7, 8
Shedding Myths vs. Facts
Myth: If hair falls with a “root,” the follicle is damaged.
Fact: The white bulb at the end is a keratinized club—not the living follicle. The follicle remains intact.
Myth: Shedding means permanent baldness.
Fact: TE is temporary and reversible in most cases, especially with proper care and trigger management.
TE vs. Other Hair Loss Conditions
Excess shedding doesn’t automatically mean TE. Other conditions can cause similar symptoms:
- Androgenetic alopecia (AGA)
- Alopecia areata
- Scarring alopecia
- Scalp Inflammation: Seborrheic dermatitis or psoriasis
That’s why it’s important to evaluate underlying health, blood work, and scalp conditions before jumping to conclusions.