A chronic autoimmune skin disorder that causes red, inflamed, scaly patches on the scalp, often leaving behind shiny, scarred bald spots. It may or may not be associated with systemic lupus.
The exact cause is unknown, but it is thought to involve a combination of genetic predisposition, environmental triggers, and autoimmune dysfunction.
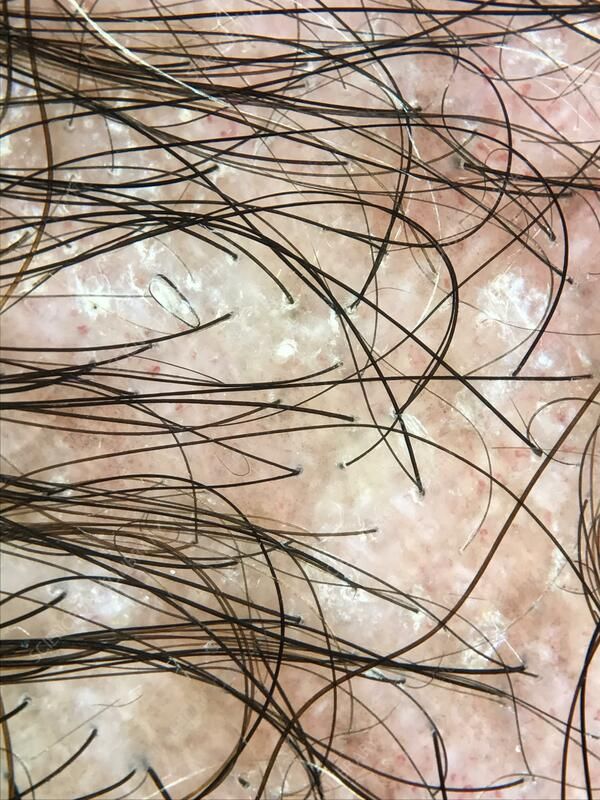
Trichoscopy shows thick adherent scales, follicular plugging, perifollicular white scales, telangiectasia, and loss of follicular openings in advanced areas
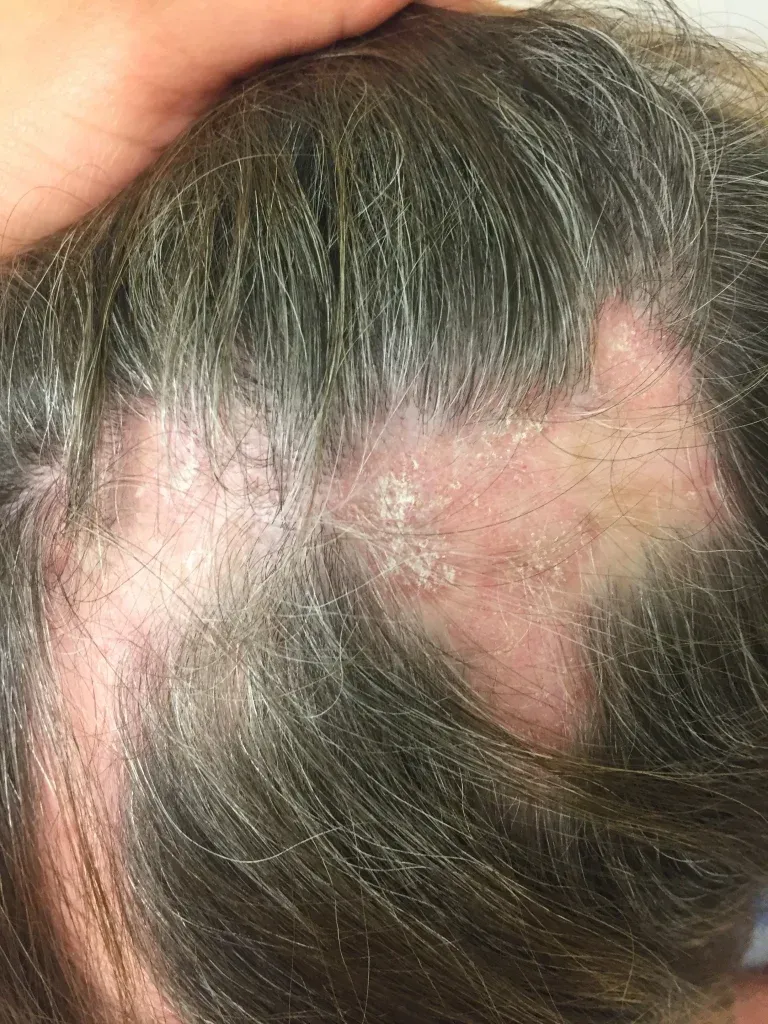
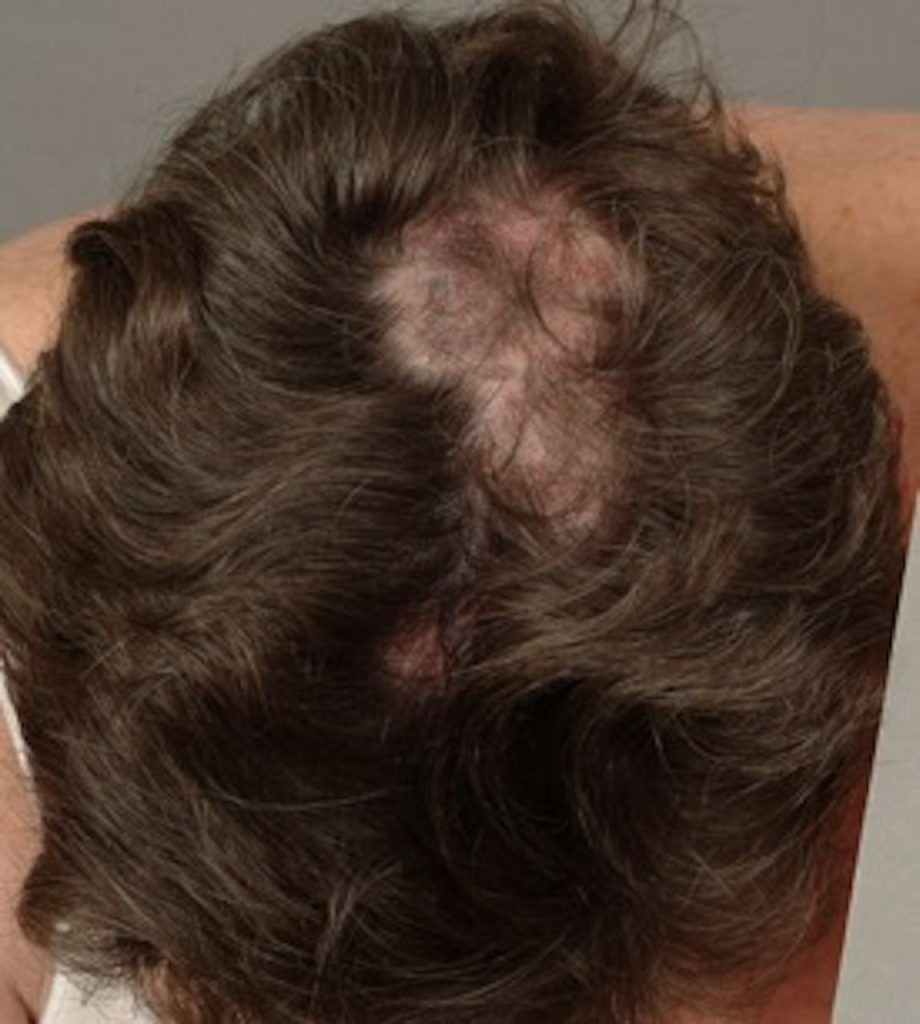
Diagnosis
Diagnosis usually requires a scalp biopsy, which helps confirm the presence of lupus-related inflammation and scarring. Blood tests may also be done to check for systemic lupus erythematosus (SLE), a more widespread form of lupus, as DLE can sometimes overlap with this condition.
Treatment Options
Consulting a dermatologist early in the disease course is vital to achieving the best possible outcome. Treatment focuses on halting the progression of hair loss and reducing inflammation.
- Topical/injected steroids
- Medication to control autoimmune activity (Hydroxychloroquine)
- UV protection – sunlight can trigger flares
- Minoxidil to support hair preservation
- Hair transplant is not advised unless stable for 2+ years and often requires a repeat scalp biopsy to ensure the disease is inactive. Transplants into inflamed areas tend to fail or worsen the disease
Prognosis
The prognosis for DLE depends on early diagnosis and effective treatment. While hair lost in scarred areas cannot regrow, stopping disease progression can help preserve existing hair.
Long-term management often involves monitoring for flare-ups and addressing any triggers. Working closely with a dermatologist is critical to achieving the best outcome and maintaining scalp health.