An inflammatory, scarring form of alopecia that often causes itching, burning, or pain along with red, scaly lesions and permanent hair loss. It’s considered an autoimmune condition.
The exact cause is not fully understood, but it is believed to involve a combination of immune dysfunction, genetic predisposition, and possibly environmental triggers.

Trichoscopy shows perifollicular scaling, perifollicular erythema, loss of follicular openings, and blue- gray dots around follicles indicating interface dermatitis.
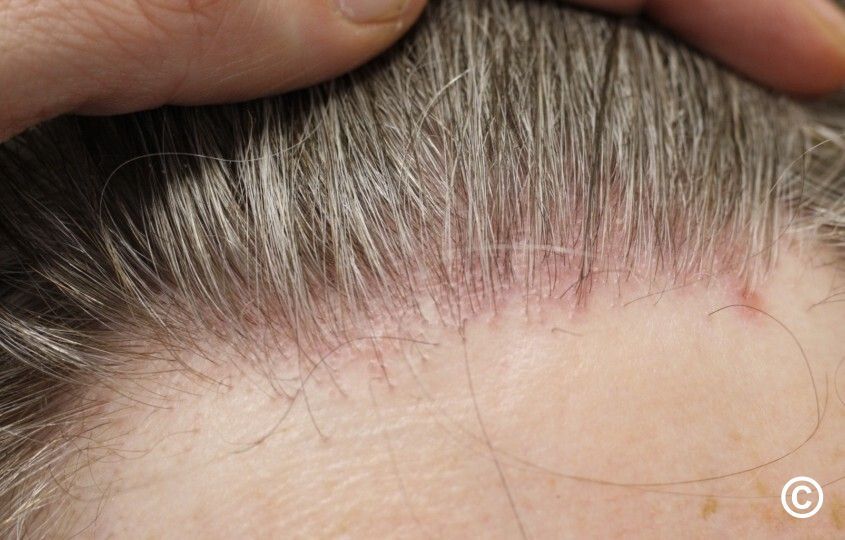
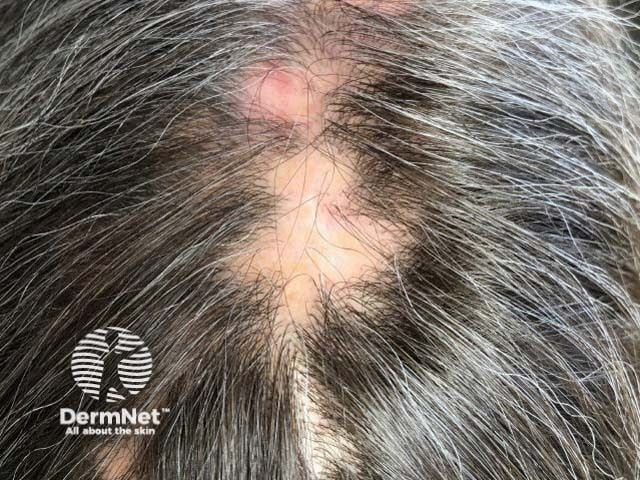
Diagnosis
Diagnosis is made through a combination of clinical examination and, if necessary, a scalp biopsy, which reveals specific signs of inflammation and damage to hair follicles characteristic of LPP. Blood tests may also rule out other autoimmune or inflammatory conditions.
Treatment Options
Consulting with a dermatologist early in the course of the condition ensures the best possible management and outcome.
- Topical/injected steroids
- Immunosuppressive medications (Hydroxychloroquine or Methotrexate)
- JAK inhibitors in severe cases
- Minoxidil to support hair preservation
- Hair transplant is not advised unless stable for 2+ years and often requires a repeat scalp biopsy to ensure the disease is inactive. Transplants into inflamed areas tend to fail or worsen the disease
Prognosis
The prognosis for LPP varies. With early diagnosis and effective treatment, it is often possible to stop or slow the progression of hair loss, though regrowth in scarred areas is not possible.
LPP can be chronic and may experience periods of flares and remission. Therefore, long-term management with regular follow-ups with a dermatologist is crucial for achieving the best outcome.